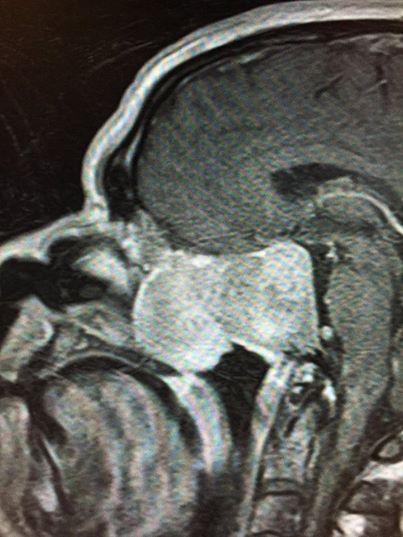
From Lewis S Blevins, Jr. MD – All too often, I see patients who come to the clinic with devastating recurrences of their pituitary tumors. For example, the accompanying MRI depicts a recurrent pituitary tumor in a patient who had had surgery 10 years prior. He had one visit with the surgeon 6 weeks afterwards. No subsequent followup was rendered and he did not undergo any testing of the adequacy of pituitary functions. He recently presented with nasal congestion and other obstruction symptoms that were worsening over a four-month period. MRI shows a rather large and dramatic tumor emanating from the sella, invading the cavernous sinuses, and extending forwards occupying half of his nasal cavity, invading the ethmoid sinuses, etc. For all intents and purposes, this tumor is behaving as if it is malignant. There are two immediate lessons to be learned. First, you should undergo surgery at a pituitary center of excellence with not only an experienced neurosurgeon but also a knowledgeable endocrinologist. Second, understand that lifelong followup is required. So, with this having been said, I would like to share with you some of my thoughts about postoperative followup.
Followup 6-8 weeks after surgery is necessary to review the MRI to determine the extent of tumor resection, plan for any additional therapy for the tumor or any hormone excesses, evaluate the adequacy of pituitary functions, to allow for replacement hormones of pituitary function is compromised, and to establish a plan of long-term followup.
Studies show that between 12 and 18% of pituitary adenomas will recur. The majority of these recurrences take place within the first 3-5 years after surgery. Aggressive tumors recur sooner. The longest time from initial surgery to recurrence of a nonfunctioning tumor that I have encountered in my practice was 30 years. Patients with hormone secreting neoplasms usually recur sooner because the hormone perturbations lead to clinical attention in patients who have previously experienced acromegaly, Cushing’s, or hyperprolactinemia. The longest time from curative surgery to a documented recurrence I have seen in a patient with Cushing’s disease was 15 years. Approximately 8-10% of patients who have Rathke’s cleft cysts will develop a recurrent cyst. Those with infected Rathke’s cleft cysts, or what are sometimes referred to as pituitary abscesses, face a 40-45% likelihood of recurrence unless they take postoperative antibiotics in which case the risk of recurrence is lowered closer to normal but is still higher than if the cyst is simple and uninfected. Patients with craniopharyngioma have a higher risk of recurrence that I would estimate to be 30-50%. Thus, lifelong followup is required and even when you think he might be rendered disease-free. I usually recommend MRI studies 6 weeks after surgery. I suggest a repeat study 6 months after surgery for those who have residual tumors when there is a concern the tumor might be aggressive or likely to regrow quickly. I recommend MRI studies one year after surgery in patients whose initial postoperative MRI shows no evidence of residual disease. Thereafter, I recommend MRI studies on an annual basis for 3-5 years for most nonfunctioning pituitary tumors. Further, I suggest MRI studies whenever symptoms of the tumor, such as abnormal visual fields or headaches, recur in a pattern that was similar to the preoperative symptomatology.
Obviously, I recommend repeat MRI studies when there is historical and physical as well as biochemical evidence of recurrent hormone hypersecretion in the setting of a history of a prolactinoma, acromegaly, Cushing’s, and hyperthyroidism.
A number of patients have seemingly normal pituitary functions about 6-8 weeks after surgery. Interestingly, however, because of the way that hormones are bound to proteins, and possibly because the pituitary gland that is compromised by a tumor or surgery which might have interrupted its blood supply may slowly fail, reassessments of pituitary and target gland hormones to assess the adequacy of pituitary function are sometimes best performed at 12 to 16 or even 24 weeks after surgery, and especially in patients who have symptoms of hypopituitarism with an onset in this time frame after surgery. Those with partial or complete hypopituitarism or diabetes insipidus are followed on a regular basis according to individual needs.
Patients with prolactinomas who have been rendered disease-free after surgery should have prolactin levels at 6 month intervals for 2 years and then annually thereafter. The prolactin should also be reassessed in the presence of galactorrhea, irregular menses, infertility, or hypogonadism. Of course, those with residual disease or recurrent disease her on a totally different plan a followup that is tailored to individual needs based on any subsequent treatment and responses to such.
Patients with acromegaly who have been rendered disease-free after surgery should have IGF one and growth hormone levels obtained every 6 months for 5 years and then annually thereafter. Primary physicians often conduct these evaluations. Referral to the pituitary center should take place for any prolactin that exceeds 20 ng/mL and especially if there are symptoms of mass effect or gonadal dysfunction.
Patients with Cushing’s syndrome who into remission usually have a period of adrenal insufficiency it lasts between 6 and 18 months. In one study, the average time patient’s had adrenal insufficiency was 10.8 months. Steroid replacement is required until normal pituitary adrenal function is resumed. Followup should be individualized and is rather complex. Generally speaking, one of the main problems I see in this group of patients is that treating physicians administer supraphysiological doses of steroids which delay recovery. I prefer replacement doses of steroids immediately after surgery. I used dexamethasone 0.25-0.375 mg daily. If I choose to use a slightly supraphysiologic dose of steroids then I do so for no more than 6-12 weeks after surgery. Periodic morning cortisol levels are obtained after patients have withheld steroids for 24 hours. Once the serum cortisol level start to exceed 5-7 mcg/dL, I consider transitioning to a shorter acting steroid, such as hydrocortisone, for one to 2 months and then we’ll perform a low dose ACTH stimulation test. If the stimulation test is normal the patient can come off steroids and we check a first, or baseline, 24-hour urine cortisol. If the response is abnormal, then we continue on low dose steroids until patient’s have a normal response based on testing in 2-3 month intervals. Once patients have discontinued steroids, I recommend 24 hour urine cortisols at six-month intervals for a couple of years and then annually thereafter. Also, the urine cortisol should be reevaluated in the time patient believes hypercortisolism may have recurred. Additional studies, such as dexamethasone-suppressed CRH stimulation tests or salivary cortisol profiles may be necessary to detect early recurrences as, in my experience, some patients recognize there Cushing’s has recurred while their urine cortisol levels are still in the upper part of the normal range.
Patients who have been treated with radiotherapy to the pituitary region should undergo testing of pituitary functions at six-month intervals for a few years and then annually thereafter because 40-80% of them will develop one or more anterior pituitary hormone deficits.
© 2014, Pituitary World News. All rights reserved.